Teams of UT faculty and Austin-area companies are crossing their fingers after submitting their proposals to Texas Health Catalyst on June 8 in hopes of being chosen as one of this year’s awardees.
“Texas Health Catalyst was based on Catalyst, a translational research program at the University of San Francisco,” program director Nishi Viswanathan said. “However … instead of supporting technologies hunting for problems to solve, Texas Health Catalyst (provides) innovators a target to shoot for.”
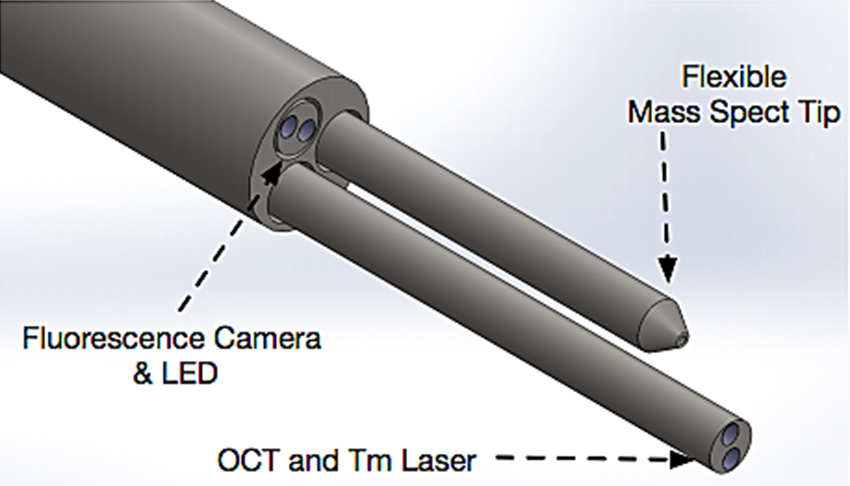
Last year, THC chose an interdisciplinary team of doctors and UT researchers that proposed a low-cost smart imaging system for minimally invasive surgery. This proposal particularly impressed the advisory panel of clinicians, entrepreneurs and Austin industry leaders, Viswanathan said.
The imaging device will aid in surgeries that typically require special training and can be extremely complex, time-consuming and even unsuccessful, according to Viswanathan. It aims to make endometriosis surgery more accurate and effective.
Endometriosis occurs when the lining of the uterus grows outside of the uterus. Pelvic peritoneal endometriosis specifically affects the endometrial tissue found in the pelvic cavity.
“(It) is a debilitating disease affecting over 7.5 million women in the U.S. alone,” Viswanathan said. “This technology … aims to make endometriosis surgery more thorough and effective.”
The advisory panel believed that this project was worth investing both time and money in, Viswanathan added.
“This project was particularly interesting to us because this team took an existing cutting-edge imaging technology they were developing for cancer imaging and applied it to a very specific pain point described in (THC’s) request for proposals,” Viswanathan said.
Although the project is still in the early stages, it is already well underway, according to biomedical engineering professor Thomas Milner.
“We are developing a suite of technologies to make intraoperative surgery safer and more effective,” Milner said.
Milner is working with Livia Eberlin, an associate professor in the Department of Chemistry, as primary investigators of the project, which combines Milner’s imaging system with mass spectrometry, a technique that can determine the composition of tissues by mass of the chemicals that make them up.
“Dr. Eberlin’s group is applying mass spectrometry to diagnose endometrial tissues, while my group is developing a low cost endoscopic imaging system,” Milner said.
The operating room is Dr. Michael Breen’s stage. Breen is an assistant professor of women’s health at the Dell Medical School and also the director of robotics and minimally invasive surgery.
“My role as a robotic surgeon is primary resection of deep pelvic wall endometriosis from surgical patients with varying stages of pelvic peritoneal endometriosis,” Breen said.
Breen said there is potential to use mass spectrometry to identify regular and atypical endometriosis during surgery.
THC looks for projects proposed by innovators who are eager to seek advice from experts and willing to incorporate these suggestions into their development plans, according to Viswanathan.
“We strive to make sure all promising technologies get the support they deserve and equip our applicants with the tools, connections and resources they need for their current and future venues,” Viswanathan said.
THC has provided instrumental support to this team, Breen said. “(It has) allowed us to focus our efforts and has helped cover the technical expenses involved with sophisticated tissue histologic evaluation … (and) mass spectrometry evaluations.”
Milner said that the new system will help improve the quality of care for women with endometriosis.
“Endometriosis is such a dreadful disease and the treatments need to improve,” Milner said. “Women suffering from endometriosis deserve … better treatment and … better lives.”