Insulin costs capped for some diabetics, UT community calls for further reform
August 26, 2022
Karley Singleton dreamed of being a filmmaker, but she said she had to push her dream to the side so she could afford insulin.
“What I want to do for my passion would be to get gigs … or work on my own sets,” radio-television-film senior Singleton said. “But I just don’t see how that can be sustainable for somebody like me who has these expenses.”
Type I diabetics produce little to no insulin, a hormone that processes carbohydrates. Both Type I and Type II diabetics take insulin to manage their condition. Over nine million Americans take insulin, according to the Commonwealth Fund.
On Aug. 16, President Joe Biden signed the Inflation Reduction Act which capped the copay cost of insulin at $35 a month for Medicare Part D patients. Currently, Texas has a $25 monthly copay cap for patients on state-regulated health insurance plans, but both people with and without health insurance — including those on federal plans like Medicaid — still grapple with high prices.
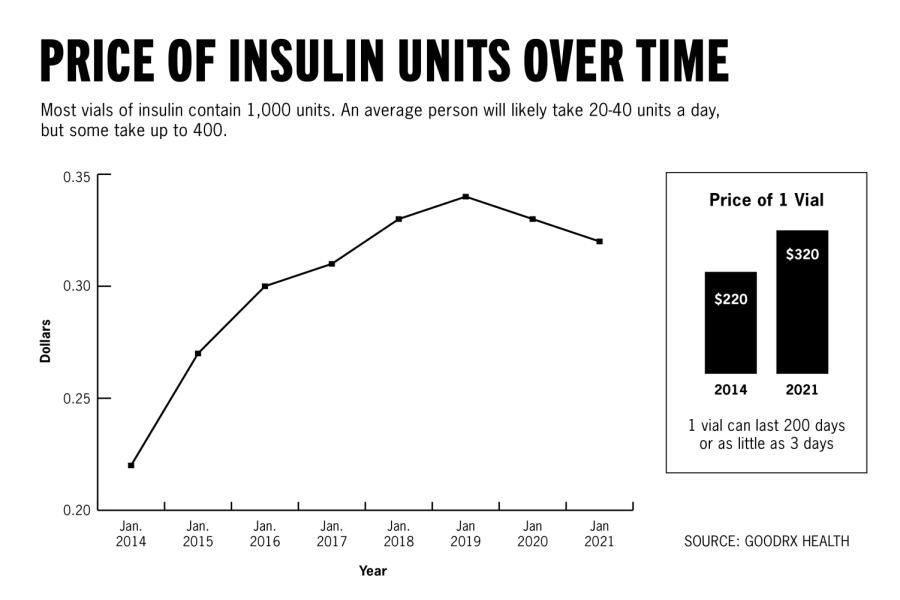
Morgan Stewart, a pharmacy clinical assistant professor, said the cheapest, often less clinically preferred insulin is $25 a vial — which for some can last as little as 10 days.
“If you’re not using insurance or coverage or any programs to help you, (it would be), ballpark, anywhere from $400 to $1,000 a month depending on your needs,” Stewart said. “Even the cheapest option out there is not cheap.”
Singleton said four vials of insulin, her supply for three months, costs $250 after insurance. She said the cost is overwhelming even with her grandparents’ support.
“Spending that much money, regardless of what the purchase is, is very jarring,” said Singleton, the social media chair for Type Texas, UT’s chapter of the College Diabetes Network. “I’ll tell my grandma how much it was for two months, three months supply and she’ll be like ‘Are you sure you need that much (money)?’ … It’s just upsetting that, yeah, I do need that much.”
Heather Cuevas, an assistant nursing professor, said some patients ration insulin to reduce personal cost, which can lead to negative health effects such as diabetic ketoacidosis which can be life-threatening.
“(If) I prescribe 20 units to someone, they may take 10 because they’re trying to stretch out the vial (and) their sugar may not be controlled as well with that,” said Cuevas, an advanced practice nurse. “It even comes down to people choosing between insulin and housing or utilities.”
Pharmacy professor Kenneth Lawson said when researchers release an updated version of the medication, it increases insulin prices, and because there is no generic insulin, patients are forced to purchase these more expensive versions of the drug. Pharmaceutical companies set the prices of insulin, which also leads to the high cost of the medication, Cuevas said.
“There’s this lack of transparency,” Lawson said. “I think (the Medicare cap) is a good step in the right direction and hopefully that can be expanded to the broader population given the nature of this medication and how critical it is.”
Cuevas said, in addition to decreasing copay prices, she wishes there was more regulation of pharmaceutical companies and insurance companies.
“I want to do what’s best for everybody that’s sitting in my office and sometimes I feel like my hands are tied,” Cuevas said. “There’s that element of ‘Why can’t this person have the best care I can give them?’ It’s not because of anything they’ve done. They need these medications.”
People who need help accessing insulin can go to insulinhelp.org for assistance and resources.